Several different names have been used to describe this condition. TCS addiction/withdrawal syndrome, topical steroid addiction and red skin syndrome all refer to essentially the same condition
What is topical corticosteroid withdrawal?
Topical corticosteroid withdrawal refers to a rare adverse reaction relating to the use of a topical steroid after it has been discontinued. This reaction can occur after prolonged, inappropriate, and/or frequent use/abuse of moderate- to high-potency topical corticosteroids. There are two distinct clinical presentations of topical steroid withdrawal:
- Red burning skin – this has incorrectly been given a variety of names, including topical steroid addiction and steroid dermatitis.
- Papulopustular (papules – a small, raised pimple and pustules – a small pus filled blister) rashes – these include steroid rosacea and perioral/periorificial dermatitis.
What is the cause of red burning skin and who gets it?
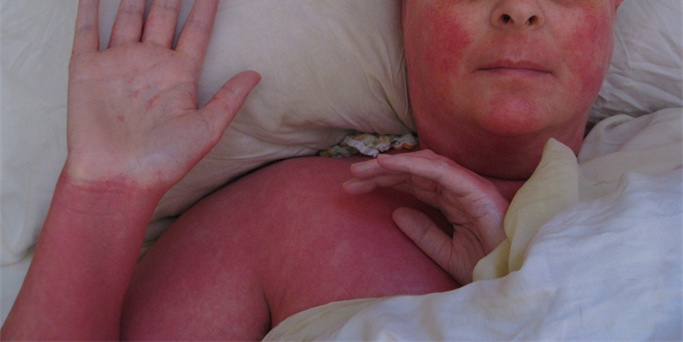
Signs of topical corticosteroid withdrawal may develop within days to weeks after stopping high-potency topical corticosteroid that has been over-used/abused — this is mostly for the treatment of atopic dermatitis.
Treatment with the topical steroid has usually been prolonged, greater than 12 months, and frequent, ie daily or more often. It has not been reported with correct use of topical steroids.
All cases reported in the medical literature of this form of steroid withdrawal have been over the age of 18 years, with a female predominance.
The overall prevalence of red skin after topical steroid withdrawal is not known, nor is it yet understood whether the lack of reported paediatric cases is due to children not being affected or to under-reporting. In a Japanese study of atopic dermatitis, 12% had poorly controlled skin disease and this group would include topical steroid-addicted patients.
What are the clinical features of topical corticosteroid withdrawal?
Before stopping the topical corticosteroid, the skin is typically normal or near-normal, although localised itch, ‘resistant’ patches of eczema or prurigo-like nodules may be present. Redness (erythema or flushing) typically starts on the face, genital area, or other steroid-treated site; in some cases this may extend to untreated sites. Early in the flare, the skin can feel quite thickened. Swelling (oedema) and papules can occur.
The usual symptom described by patients is burning and/or stinging. Itch may also be reported, especially once the redness starts to fade and the dry scaly (desquamative) phase begins. Patients often report skin sensitivity, including intolerance to moisturisers and environmental factors. Excessive sweating and itchy weals are a sign of recovery.
One of the difficulties is determining whether the skin reaction observed is due to the stopping of topical corticosteroids, or is simply a worsening of the underlying skin disease for which the topical steroids had been prescribed.
Complications of topical corticosteroid withdrawal
Patients with red burning skin after topical corticosteroid withdrawal may be distressed by the intensity of itch, lack of sleep, and difficulty in treatment. They may also develop a secondary infection.
How is topical corticosteroid withdrawal diagnosed?
The definition of topical corticosteroid withdrawal requires the following features to be present:
- A rash that has appeared within days to weeks of discontinuing topical corticosteroid that has been used for many months. This flare may be worse than the pre-treatment rash.
- The rash must be only where the topical corticosteroid was being applied, at least initially, although it can later spread more widely.
A flare of the underlying skin disorder such as atopic dermatitis/eczema can be difficult to distinguish clinically. Topical corticosteroid withdrawal should be considered if:
- Burning rather than itch is the main symptom
- The redness is confluent rather than patchy
- The rash resembles atopic dermatitis/eczema but involves unusual sites and is ‘different’
- There has been a history of continuous prolonged use of mid- or high-potency topical corticosteroid (greater than 1 year).
A skin biopsy is generally unhelpful to distinguish from a flare of the underlying skin disorder.
Patch testing may identify some cases of contact allergy to the topical agents being applied to the skin, eg topical corticosteroid or other topical medications, moisturisers, cosmetics.
What is the treatment for topical corticosteroid withdrawal?
There is no agreed treatment for topical corticosteroid withdrawal, apart from ceasing the topical corticosteroid. However, whether this should be tapered or abrupt has not been determined. Japanese reports suggest there is minimal difference in the outcome, so recommend immediate cessation. A tapering course of oral steroids is helpful, as the addiction appears to relate only to the use of topical corticosteroids.
Management
Supportive measures are recommended for physical and psychological symptoms. Patients can trial oral antihistamines for their itch. Burning pain may be alleviated with ice or cool water compresses or possibly nerve pain medication. Sleeping aids and anxiety medication may be appropriate in some cases. Oral immunosuppressants and light therapy have been reported to help selected patients. Calcineurin inhibitors and a tapering course of oral antibiotics (eg doxycycline, tetracycline and erythromycin) have been found helpful in preventing and treating secondary infection.
How can topical corticosteroid withdrawal be prevented?
Prevention is best, with patients and doctors being alert to the risk and avoiding prolonged frequent and prolonged use of moderate to high potency topical corticosteroids. The higher the potency, the longer the period of application (ie more than one year), and the more frequent the application (more than once daily), the more likely that topical corticosteroid withdrawal may occur. Concerns about the risk of topical corticosteroid withdrawal should not prevent appropriate management of atopic dermatitis/eczema with topical corticosteroids, as far more people respond to appropriate topical corticosteroid use than develop a withdrawal rash.
What is the outlook for topical corticosteroid withdrawal?
The duration of acute topical corticosteroid withdrawal and time to peak is variable from days to months, before eventually the skin becomes ‘normal’. It can take weeks to years to return to its original condition.
SOURCE: Hopes relief
This information was obtained from DermNet NZ & The Royal Australian College of General Practitioners
It is not the policy of the Eczema Association of Australasia Inc to recommend or endorse any product or treatment.
It is part of the role of the Association to provide information on a wide range of products and treatments to keep those involved with eczema as fully informed as possible as to all options available. For medical advice, consult your health professional.











← Older Post Newer Post →